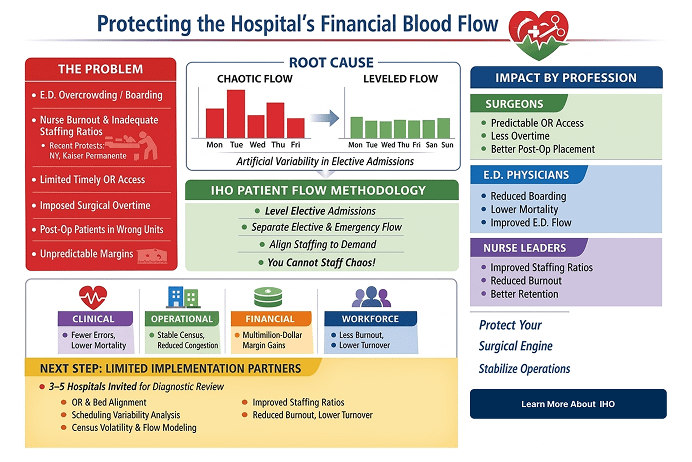
Nurse Staffing
Optimized staffing enhances patient care and reduces nurse burnout.
Physician Staffing
Effective staffing improves patient care quality and reduces delays.
Readmissions
Reducing readmissions through effective discharge planning and coordinated follow-up care.
Inpatient Mortality
Focus on early interventions to reduce inpatient mortality rates.
Patient Safety
Prioritize safety to minimize errors and enhance patient trust.
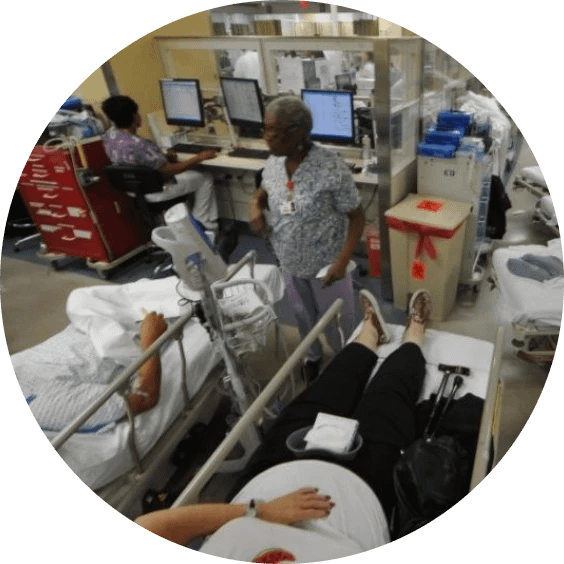
Boarding and Diversion
Improve patient flow to reduce emergency care delays.
Hospital Overcrowding
Efficient management reduces overcrowding and enhances care delivery.