Artificial Variability
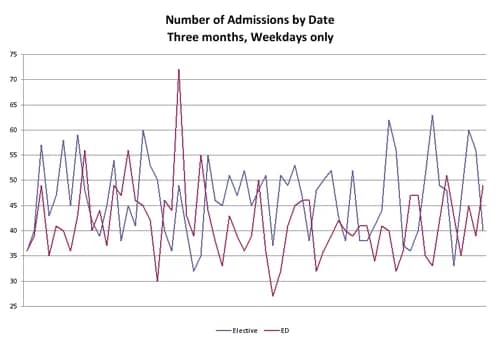
The flow of patients through the healthcare delivery system varies for two reasons – natural and artificial. The flow of Emergency Department (ED) patients is an example of natural variability. The reason ED flow is naturally variable is because the timing of patients’ arrival is primarily driven by the timing of sickness, which is naturally occurring. As compared with ED flow, the variability in the flow of elective scheduled patients is primarily artificial in nature and driven chiefly by scheduling practices. The magnitude of this artificial variability in elective flow often surpasses the natural variability in emergency department flow and wreaks havoc on the healthcare delivery system, particularly in hospitals. Take a look at the below chart showing one hospital’s emergency and elective scheduled admissions over a three month period and notice how the day to day variation in the two is almost comparable.
Artificial variability leads to unnecessary competition between elective and emergency patients resulting in
- Rejections, delays and cancellations
- Decreased quality of care and patient safety
- Decreased patient, staff and provider satisfaction
- Increased system-wide stress and waste
- Decreased throughput (i.e. number of patients), revenue, and patients’ access to care
- Increased healthcare cost
Artificial variability has negative effects for patients, providers and payers alike.
To address artificial variability, and to employ the science of Operations Management to design healthcare operations, faculty of the Institute for Healthcare Optimization developed an approach to manage patient flow variability. Artificial Variability and IHO’s recommended approach are described in great detail in Joint Commission Resources’ second edition of Managing Patient Flow in Hospitals: Strategies and Solutions and in the guidance document prepared for the California Healthcare Foundation.